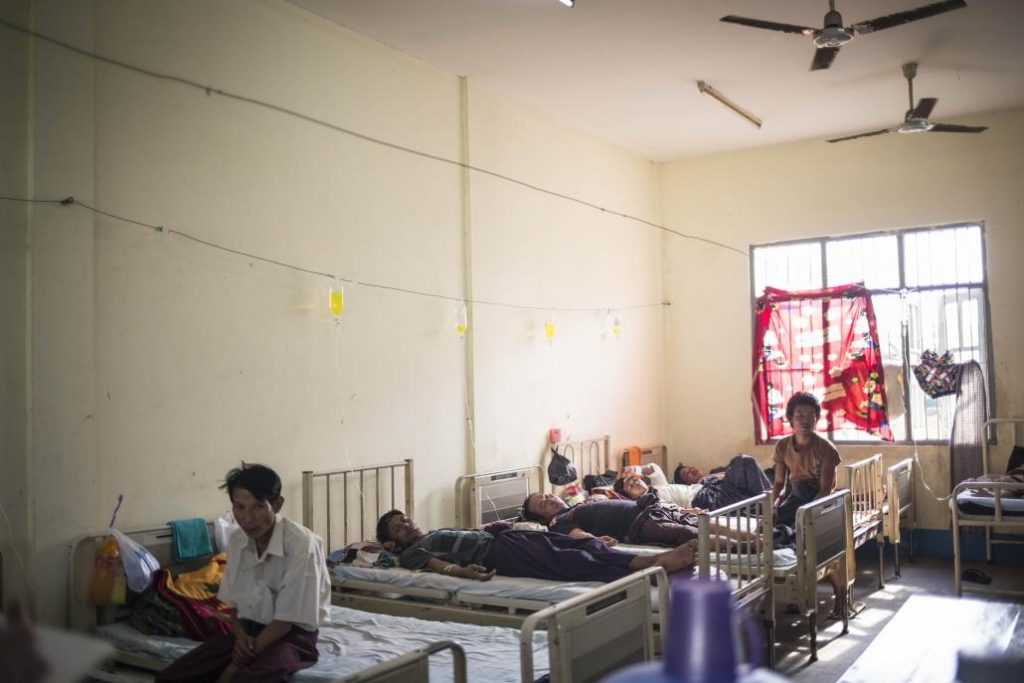
The ready availability of cheap alcohol has created a national problem that Myanmar’s underfunded public health system is having difficulty addressing.
In the war-torn western Myanmar state, small-scale distilleries are meeting a rising demand for cheap alcohol, but the spread of brewers is reducing profits while lack of regulation is sparking a health crisis.
BY Frontier