After 70 years of conflict, the KNU and local NGOs are beginning to work alongside the government in providing healthcare to the Karen people.
By JARED DOWNING | FRONTIER
Photos NYEIN SU WAI KYAW SOE
A cycle crash and a nasty gash brought Nant Aye Cho to Thailand.
With a bleeding foot and toddler in tow, the Pwo Karen woman made her way down the mountain trails to the government hospital in Kawkareik, Kayin State, only to find that the doctor was out running errands, or possibly at lunch—it was difficult for her and her husband to understand the hospital staff, who were less than thrilled to deal with a few village walk-ins who couldn’t even speak Myanmar.
Figuring she probably couldn’t afford the hospital fees anyway, Aye Cho decided instead to cross the shallow Moei River to Mae Sot, Thailand and check into the Mae Tao Clinic, a free health centre for migrants and refugees.

Nyein Su Wai Kyaw Soe | Frontier
Support more independent journalism like this. Sign up to be a Frontier member.
As Aye Cho related her journey – her words translated first from Pwo Karen to Sgaw Karen, and then into English – nurses and medics swirled around the main ward at Mae Tao, treating patients in wheelchairs and on pallet beds.
Some seeking treatment had lived on the Thai side of the border for years, even decades. Others, like Aye Cho, couldn’t afford or access the government hospitals, or didn’t trust them.
The Mae Tao Clinic, established in 1989 to serve refugees from conflict-ridden Kayin State, remains the de-facto public hospital for the estimated 250,000 living under Karen National Union authority.
This is despite the Myanmar government’s desire to expand the tentacles of the state – including provision of health and education – into newly peaceful areas of the country, and recent funding cuts by donors.
The Mae Tao Clinic in Thailand. (Nyein Su Wai Kyaw Soe | Frontier)
As a result of the 2015 nationwide ceasefire, the government and its long-time foe should theoretically be able to cooperate to treat people within Myanmar’s own borders. Indeed, the Ministry of Health and Sport identifies “ethnic health organisations”, or EHOs, as essential for its goal to achieve universal healthcare in five years.
But the effort must first overcome a mire of bureaucracy, data gaps, language barriers, old prejudices and endless meetings on how to move forward. And even before progress can be made with the government, an accord must be struck within the ensemble of independent Karen EHOs, which include DKBA Healthcare, the Karen Peace Force, the Burma Medical Association, the Back Pack Health Worker Team and several other organisations.*
Most of these have agreed to join the aegis of the largest Karen EHO, the Karen Department of Health and Welfare.
In the meantime, though, many in rural Kayin rely on scattered triage sites or the Mae Tao Clinic for their healthcare needs.
Health in the hills
To call the KDHW village tract health centre at Thar Yar Gone village a “clinic” is a bit of an overstatement.
The concrete building is in a grey area between the Myanmar government and KNU administrations. Other than basic aid and medicines, its medics and volunteers mainly provide transport and referrals to other hospitals for the roughly 1,000 villagers in the area.
Most of the day’s patients arrive in the morning on motorbikes or cattle carts, seeking treatment for dysentery, aches and pains. But their ailments are not always so mild.
Clinic director Saw Eh Say described one appendicitis patient who came in four days before Frontier visited.
“The man was so severe that we referred him to the Kawkareik Township Hospital, but on the way he passed away,” Eh Say said.
That tragedy was more the fault of the narrow trails that link the village tract to the outside world than the clinic’s resources. However, Eh Say spoke about another patient, a woman with a severe uterine infection, who actually made it to the government hospital, to little avail.
According to Eh Say, the staff at the hospital grumbled, asking why the KDHW couldn’t care for its own patients, and were reluctant to process her. He claimed they gave her minimal treatment and refused to do more – even when the woman’s condition grew worse – unless she paid hefty fees.
In the end, they simply took her to the Mae Tao Clinic.
“[Previously], the Kawkareik township medical officer said he will follow up with his staff to collaborate with my clinic and other health centres, but nobody obeyed him,” Eh Say said. “I don’t know the reason why they don’t want to work with us.”

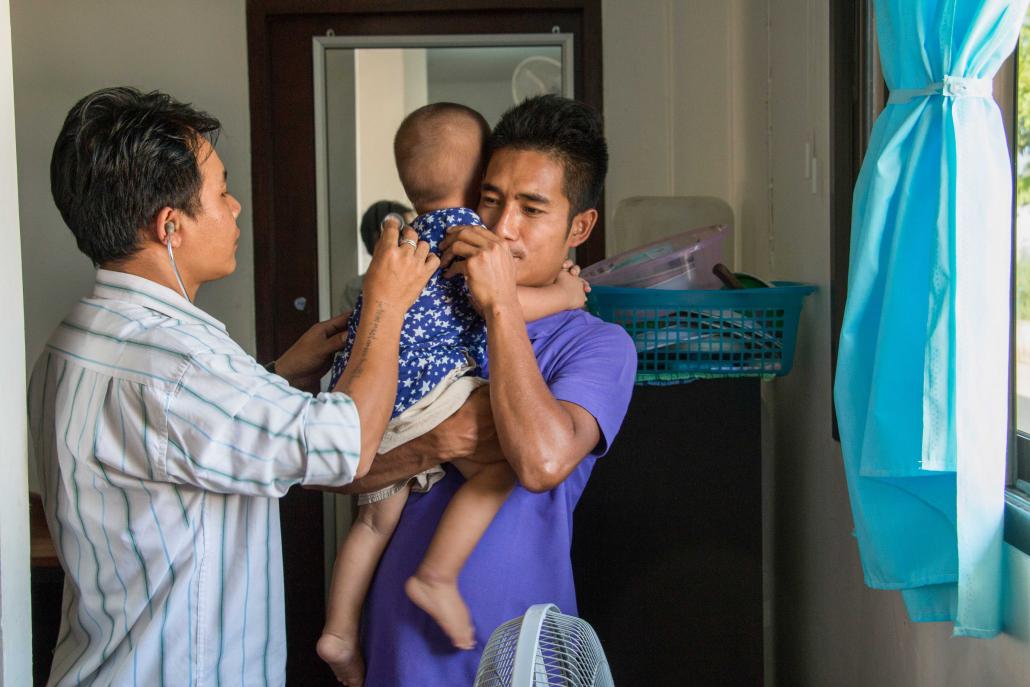
Nant Aye Cho came to the Mae Tao Clinic after first seeking treatment for a foot injury at Kawkareik Township Hospital, where there was no doctor available. (Nyein Su Wai Kyaw Soe | Frontier)
Eh Say was unwilling to speculate on the reason for the lack of cooperation. It doesn’t really matter, he said, because in the end it all comes down to money: Good treatment is rarely free, and rural Karen people can rarely afford it.
Thus, crossing into Thailand remains the default healthcare option. One middle-aged man, who was visiting the clinic to get pain medication for his back, told Frontier that in his community nobody considers options other than Mae Tao when they break a bone or come down with dengue fever. The clinic is free, there are Karen-speaking staff and Mae Tao is only an hour further than the Kawkareik Township Hospital.
The Mae Tao Clinic has 140 beds and can refer cases to the 400-bed Thai public hospital in Mae Sot, which devotes almost half of its capacity to migrants, according to Mae Tao’s data. But the days of a single health centre shouldering the Karen burden may be numbered.
Intensive care for policy
With democracy and tentative peace, the waves of battered refugees have ebbed – along with funding for humanitarian programs along the border.
Even though patient numbers at Mae Tao have remained steady, donor contributions have declined by as much as 70 percent, said Dr Cynthia Maung, who founded the clinic for fresh waves of refugees following the nationwide uprising in 1988.
Instead, donors are prioritising “development” projects inside Myanmar’s borders.
“The population is growing and the ratio of health workers and doctors, nurses in Thailand or Burma, especially in the border area, has become a big challenge,” Cynthia Maung told Frontier.

Mae Tao Clinic founder Dr Cynthia Maung says the clinic’s funding has dropped as much as 70 percent but patient numbers remain steady. (Nyein Su Wai Kyaw Soe | Frontier)
With dwindling healthcare resources on the Thai side of the border, Cynthia Maung said Mae Tao has had to increase referrals to hospitals in Myanmar. But matching, say, an HIV patient with a government hospital, communicating the specifics of their condition and treatment history to the staff, and ensuring that they continue to receive proper care can be a herculean task.
“The problem is that many young people are working in Thailand and moving back and forth,” she said. “Thirty percent don’t have a national identity card.”
It is common for people from Kayin State to arrive at a hospital with no identification, or an ID document that is recognised by one of the KNU organisations but not the Myanmar government. Even the name of their township might not match up. The area known as “Hpa-Ann” to the KNU, for example, also contains what the Myanmar government recognises as the Kawkareik, Myawaddy and Hlaingbwe townships.
“In the hospital you need referrals for continuity of care and quality of care,” Cynthia Maung said. “[Otherwise] there is no consistency of care.”

The Karen National Union’s Karen Department of Health and Welfare runs a small clinic in the village of Thar Yar Gone, which is in a grey area between the government and KNU administrations. (Nyein Su Wai Kyaw Soe | Frontier)
She fears that until the various administrations can develop and merge their systems, a child with dengue fever, a farmer with a broken leg or a woman going into labour might find themselves languishing in a waiting room as the red tape is sorted.
Fortunately, some progress has been made in recent years, if mostly in meeting rooms rather than hospital wards.
KDHW recently opened its third medical staff training centre in government-controlled Kawkareik, and democracy and the subsequent ceasefire have allowed NGOs working in KNU territory – formerly holed up in Mae Sot offices – far greater levels of access.
Furthermore, most of the various Karen healthcare providers have at least agreed to operate under the same umbrella, there have been initial meetings with Myanmar’s Ministry of Health, and the KDHW has initial drafts a five-year healthcare plan that mirrors that of the Myanmar government.
Eventually, in an ideal world, the Ministry of Health and KDHW would have complimentary registration and referral systems, the ministry would send doctors to KDHW clinics, and the Myanmar government would provide some funding and resources.
“It is not only government money,” said KDHW director Saw Eh Kalu Shwe Oo. “It will also need donation money and international assistance money, so those [parties] need to look to the national health plan and also the federal Kayin State health plan.”
Yet the issue of funding remains a future bridge to be crossed. At the moment, the KDHW plan is mainly a statement of priorities and goals; anything more detailed and action-oriented would need both Ministry of Health accreditation and backing by the various organisations under the KDHW umbrella.
Some organisations, such as the Back Pack Health Worker Team, also have operations in neighbouring states, and are thus accountable to not only Karen, but also Mon or Shan groups for their policy decisions.

Nyein Su Wai Kyaw Soe | Frontier
Furthermore, some Karen groups are simply less trusting of their former adversary of 70-years, fearing that the government will use healthcare cooperation as a way to chip away at their hard-earned sovereignty.
Even if they trust the Ministry of Health, Eh Kalu Shwe Oo explained, they may not trust the Tatmadaw, national parliament or other stakeholders.
As for Cynthia Maung, she does not mistrust the Myanmar government as much as the idea of aligning too closely with the Ministry of Health’s broad, nationwide plan.
She argued that the top-down approach diverts resources from the organisations and projects in the trenches, citing Mae Tao’s own ebbing resources but steady intake of patients.
“Thailand is looking at a national health plan, and Burma is looking at a national health plan, but border health is a more regional approach,” she said. “Sometimes the national health plan, coming from the top, it is not appropriate or relevant to local context.”
Eh Kalu Shwe Oo, at least, tends towards optimism, and he assures hesitant parties that the way forward is towards true federalism. He uses an analogy coined by KDHW director of policy Dr Phu Marta – that of a fabric of many coloured strands, together strong and effective, but each strand retaining its own identity and mindful of its unique needs.
Perhaps in five years or so Aye Cho and her family will start going to her local hospital. For now, she will keep crossing the river.
*Correction, November 28: An earlier version of this article erroneously referred to the Border Guard Force as an independent Ethnic Health Organisation.







