The care available in Myanmar to treat mental illness is well-established and widespread but heavily focused on psychiatry and is only beginning to catch up with modern standards of treatment.
By JARED DOWNING | FRONTIER
THE DEPRESSED teenager who was referred to Dr Ohn Hlaing, a psychologist, received the best possible care.
The boy had been struggling in a new school, was retreating into himself and talking about giving up his studies. When his family sent him to a mental health clinic in Yangon, a psychiatrist diagnosed him with depression, but, believing that drugs were not the best option, referred him to Ohn Hlaing for counselling and therapy.
It was an ideal scenario, a dialogue between family, a doctor and a therapist that led to effective, individualised treatment. As a response to mental illness, it was also a scenario unavailable to most Myanmar people.
There is a system in Myanmar for treating anxiety, depression, addiction, psychosis and other mental illnesses, but it is a study in contradictions: mental health has been a part of the state healthcare system since the 1970s, but little research has been conducted on the prevalence of mental health problems among the population. The most recent extensive report on mental health in Myanmar was published by the World Health Organization in 2006.
Support more independent journalism like this. Sign up to be a Frontier member.

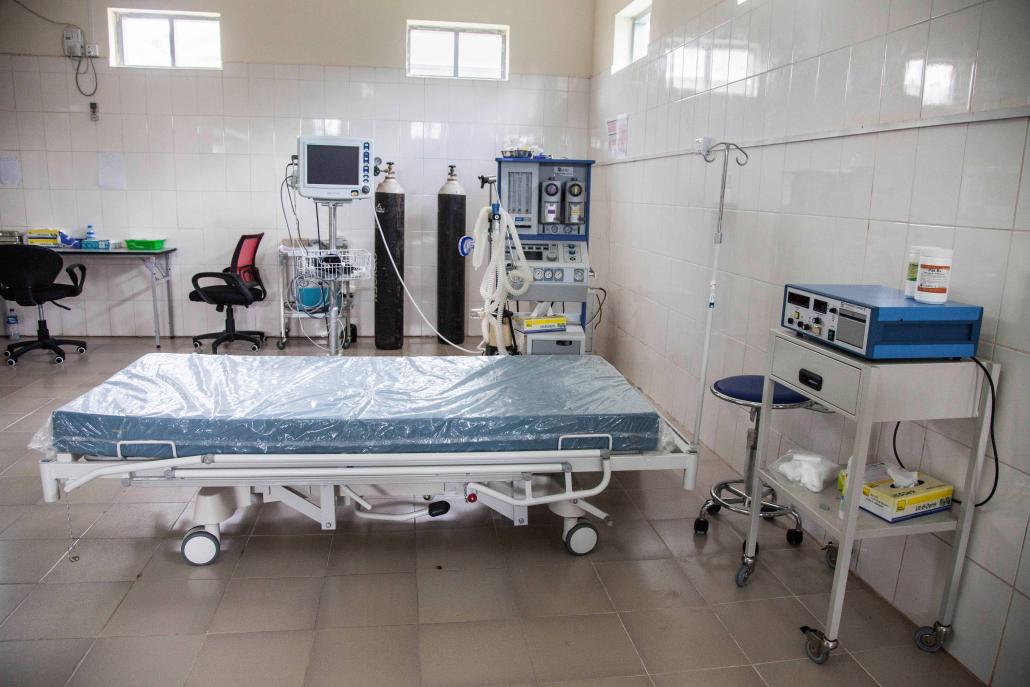
Female patients at the mental health hospital in Yangon. Myanmar has two mental health hospitals, as well as mental health wards in general hospitals throughout the country. (Theint Mon Soe — J / Frontier)
Despite the presence of in-patient and out-patient facilities throughout the country, the Myanmar Mental Health Society claims that only one person in ten receives the treatment they need.
Myanmar has hundreds of practising psychiatrists, but the number of psychologists can be counted on the fingers of one hand. (Psychiatrists are specialist doctors who often treat their patients with medication, whereas psychologists use counselling, behavioural therapy and other non-medical techniques.)
The treatment gap
There are two designated mental health hospitals in Myanmar; one each in Yangon and Mandalay. There are also 70 drug treatment centres nationwide and mental health wards at hospitals in all 14 states and regions. Treatment is affordable for many. A consultation with a psychiatrist in private practice costs about K5,000.
Psychiatric medication, too, is relatively affordable, said psychiatrist Dr Soe Min, general secretary of the Myanmar Mental Health Association. He said some top-tier medication is not available in Myanmar, but patients have access to a wide variety of drugs. He prefers a few brands of medication imported from India that have been approved by Myanmar’s Food and Drug Administration.
Although the FDA has struggled to prevent substandard or counterfeit medication being imported from China, Thailand and India, it will be a long time before Myanmar can produce its own psychopharmaceuticals.
The Yangon Mental Health Society estimates the treatment gap for mental illness to be between 85 and 90 percent. In other words, only 10 to 15 people in every 100 receive the care they need.
Access to treatment can be limited, said Dr Tin Oo, head of psychiatry at Yangon University of Medicine. He said that Myanmar has only one working psychiatrist for every 260,000 people, and they tend to work in urban areas.
Nevertheless, Dr Win Aung Myint, an officer in the Yangon Mental Health Society, said the real issue is not accessibility, but people not seeking treatment.
“As a developing country, we are increasingly producing the manpower, especially in psychiatrists,” said Win Aung Myint, who advises the Ministry of Health. “We have treatment, but the public doesn’t utilise it.”
jtms-mentalhealth-10.jpg
Electroconvulsive therapy equipment at the Mental Health Hospital in Yangon. (Theint Mon Soe — J / Frontier)
One of the biggest obstacles to treating mental health patients is stigma and fear of discrimination, said Win Aung Myint.
“People believe [those with mental illness] behave very strangely and are unpredictable and dangerous, so they don’t want to tell others, ‘I have a brother or sister who is suffering a mental illness,’” he said.
The problem, which is not specific to Myanmar, remains one of the greatest barriers between those with mental illness and the treatment they need. People may not even recognise that they have a mental illness, and if they do, they may fear being labelled ayoo, which means “crazy” or a “fool”. Their image of treatment may not differentiate between a light regime of antipsychotic drugs and being strapped to a hospital bed.
Happiness, over the counter
This apprehension may not be entirely unwarranted, said Dr Hannah Kyaw Thaung, an Irish-Myanmar psychologist who co-founded Marble Psychological Services in Yangon.
“If you move from the [general practitioner] up to the psychiatrist, then you are immediately crazy. The word crazy in Burmese is still used, and that’s what you are when you go to the psychiatrist,” she told Frontier.
Hannah Kyaw Thaung is a clinical psychologist, not a psychiatrist. She might counsel a teenager to develop strategies for breaking depressive thought patterns, or help a woman deal with a traumatic experience by inviting her to tell it as a story.
Unfortunately, psychological treatment is extremely rare in Myanmar. Hannah Kyaw Thaung is one of only five practising clinical psychologists in the country.
Because psychiatrists carry the burden of providing most mental health care, the result can be fast diagnoses that may not necessarily be accurate. They might make a list of basic symptoms, find a close-enough match in the Diagnostic and Statistical Manual of Media Disorders published by the American Psychiatric Association or the WHO’s International Classification of Diseases, and send patients to a pharmacy or the psychiatric ward.
Treatment in Myanmar is based on a well-established “medical model”, Hannah Kyaw Thaung said, “and they are using that in mental health”.
This means that although mental health services are extensive, they may respond to complex psychological conditions no differently than they would to arthritis or hypertension.
“You get stuck in that system,” said Hannah Kyaw Thaung. “There is no stepping down. If you do become better and have the right support and are feeling better, there’s no system to get tiered back down. So people get stuck in hospital and they get stuck in treatment.”
She has heard of patients who took the same medication for ten years or more and suffered long-term side effects worse than the initial illness.
The system can be especially dangerous for children, said Dr Sjoukje Zjilstra, clinical child psychologist at Marble Psychological Services. Parents want quick, straightforward fixes for their children’s emotional and behavioural illnesses free of any unpleasant labels, she said.
jtms-mentalhealth-35.jpg

Theint Mon Soe — J / Frontier
“They wish to fix it now rather than tomorrow, so [the child] goes through a rapid assessment and then receives medical treatment. They see the treatment isn’t working … so then through other channels, maybe the school, they arrive at me,” Zjilstra said.
“Unfortunately, unless you have people who are trained, it’s easier to put people in hospitals than to treat them in the community,” said Hannah Kyaw Thaung.
Sometimes people suffering from paranoia or neurosis are shunted into hospitals for the mentally ill where they are surrounded by strangers and other patients and at risk of a further deterioration in their condition. The prospect of being admitted to hospital deters many people from seeking treatment, said Hannah Kyaw Thaung.
Mind and body
Of the five clinical psychologists in the country, only three are Myanmar-born. They include Ohn Hlaing, the head of the Myanmar Psychology Association. After completing a PhD in Britain in 1969, he was conscripted into the military during the Ne Win era to perform psychological evaluations of new officers. In his current role, he rotates between hospitals and clinics in Yangon, working with the resident psychiatrist.
“[The psychiatrist] usually sees the patient first, and if he thinks there is a real [medical] problem, he takes it on himself. If he thinks it is milder or different, he refers to me, and I start doing a more thorough interview,” Ohn Hlaing told Frontier.
The teenaged boy referred to Ohn Hlaing was depressed because of events he’d experienced. At first, Ohn Hlaing simply listened, allowing the boy to speak freely about the events and how they affected his feelings. Then he discussed the nature of the boy’s problems and advised how he could respond more positively to his situation.
Another of Ohn Hlaing’s patients was a man who had raised a family and worked in the same job for years before suddenly, and without any apparent reason, losing motivation, feeling constantly tired and having suicidal thoughts. Ohn Hlaing sent him back to the psychiatrist for medical treatment.
Unfortunately, such cooperation between psychologists and psychiatrists in Myanmar is extremely uncommon. Although Yangon University has a psychology program, it cannot produce clinical psychologists, and students trained abroad often never return or find themselves ill-prepared to treat Myanmar people when they do.
“In the West, it is much more formal. The way they talk is very formal. Our people are very informal. They can’t express what they feel,” said Ohn Hlaing. “It is the technique of communication, not the technique of psychology. To be connected to what the other is feeling. But when people are working for so long in other countries they are much more connected to people there, not their own people.”
Religion plays heavily on the Myanmar psyche, said Ohn Hlaing, who describes himself as an observant Buddhist. A man might think his anger management problem is due to excessive greed or another vice rather than unhealthy cognitive-behavioural patterns and seek help from a monk rather than a therapist, he said.
Ohn Hlaing incorporates Buddhist tenets into his treatment. “This is the culture. You can’t delete these things. They are born with these things,” he said. Yet the Myanmar paradigm might not come as easily to a young psychologist trained exclusively with Western techniques and Western clients.
Despite being a psychiatrist, Win Aung Myint agrees that treatment options are too limited.
“In our country we cannot produce clinical psychologists on our own, only psychiatrists. Clinical psychologists are very lacking,” he said. “Now we are trying to [introduce] the diploma in clinical psychology at Yangon University. We have a lack of resources and it is a great challenge for us, but we have to [offer the diploma] because the important role of clinical psychologists in our country.”
Mental health mentality
The response should go beyond psychiatrists and psychologists, said Hannah Kyaw Thaung. GPs, social workers, teachers and others should be trained to become mental health first responders, an approach she called “multidisciplinary care”.
“Then the client has full team, not just one person thinking about their background. And that’s what definitely missing in the system. We all operate in a very isolated manner.”
Win Aung Myint said community attitudes towards mental health are slowly changing for the better, thanks partly to mobile clinics that tour rural areas and the introduction of workshops that train GPs and nurses to recognise mental illnesses and provide basic treatment.
Yet, many Myanmar prefer to isolate and compartmentalise their mental health issues, said Ohn Hlaing. Indeed, he said, people often forgo more nuanced treatment options even when they are available. They prefer to think of their mental illness as a straightforward disease rather than as a part of who they are.
“They don’t want to accept that they are psychologically weak. They even hide the problem,” Ohn Hlaing said.
The new generation
Mental health care seems to be improving, gradually.
Psychiatrists and psychologists gathered in Yangon in late September for the fourth Myanmar Mental Health Conference, held under the theme: “Change: The way forward to achieve better mental health services”.
Topics discussed at the event included expanding mental health services in schools and increasing access to care in rural areas. Specialists from Japan, Britain and the United States gave presentations on community-based mental health and better psychological monitoring for workers.
Participants at the event included Dr Win Thaung Min and Dr Naing Myat Kyaw, who are interns at Yangon Mental Health Hospital. By the time they become licensed psychiatrists and begin their mandated government service, they will have spent 10 years at university. Their starting salary will be K250,000 a month.
“Something we have to ask ourselves is, why we are doing this work for this salary?” said Win Thaung Min. “We want to help people. In our country, we need mental health services. We have to change. We have to change the script and the mindset of the people,” he said.
But students with Win Thaung Min’s passion for mental health are difficult to find, said Tin Oo.
“In Myanmar psychiatry is not popular subject,” he said, adding that the enrollment for psychiatry students is only about 30 a year. “So we need more psychiatrist for mental healthcare, and more [general practitioners] are needed to train for basic mental healthcare.”
Naing Myat Kyaw is unfussed about the low starting pay. “Our people need more psychiatrists and more mental health doctors,” he said. “I enjoy working with patients at the hospital. I can hear what they think and feel what they feel. I can learn with them, and I am very happy.”







