Pharmaceutical products being packaged for sale in a pharmacy in downtown Yangon. (Ann Wang / Frontier)
The first private sector drug companies are poised to begin production, easing Myanmar’s reliance on imported pharmaceuticals.
Progress Biochem’s new drug making factory looks as if it belongs in the International Space Station, not among the warehouses and smokestacks of Yangon’s industrial outskirts.
The company’s chief executive officer, U Htoo Myint, didn’t try to contain his pride when he showed off its immaculate white corridors, glittering steel machinery, World Health Organization-standard laboratory and Myanmar-born architects and engineers.
All the factory needs to begin making Myanmar’s first privately-produced medicine is a licence.
For the last half century, a handful of state-owned factories – and one public-private joint venture – have produced Myanmar’s meagre pharmaceutical output. All other pharmaceutical products – between 80 percent and 90 percent – are imported, either from reputable international companies or bargain-bin producers that slip substandard or phony medication past the Department of Food and Drug Administration, the FDA.
Myanmar is trying to kick its foreign drug habit: In recent years the government has offered incentives to seven private distributors to try their hand at manufacturing domestically. They include local and international outfits, and their first factories are nearly ready to begin producing what will theoretically be affordable yet high-quality medication.
Support more independent journalism like this. Sign up to be a Frontier member.

The entrance to the BPI Pharmaceutical Factory in Yangon’s Insein Township. (Ann Wang / Frontier)
Needles and snakes
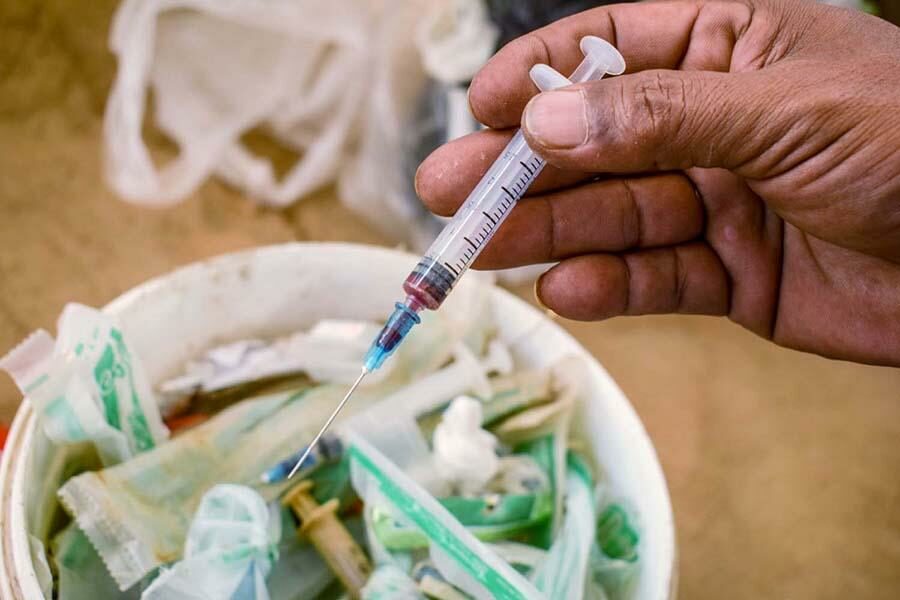
The state-owned BPI Pharmaceutical Factory in Yangon’s northern Insein Township could be a military base. Medicine has been produced in the gated, sprawling compound since 1954 and it is the only facility in the country making finished biological products, such as antibiotics, vaccines and antivenom, for snake bite.
Still, the plant only produces two of the eight vaccines in Myanmar’s national immunisation regimen: hepatitis B and tuberculosis Most of the country’s vaccines and antibiotics come from beyond its borders, mostly from international non-government organisations, such as the GAVI Vaccine Alliance.
“Myanmar is currently an LDC country, ‘least-developed country,’ so it receives this support,” said Dr Aung Zaw, head of quality assurance at the Insein factory and one of the inspectors of the private plants.
The trouble with this arrangement, he said, is that it depends on Myanmar’s ‘least-developed’ status. He worries that the country is developing faster than its capacity to provide these medicines, which could leave Myanmar with a shortage if the international aid dries up.
Nevertheless, the new manufacturers will not be allowed to produce vaccines, antibiotics, antivenom or other injected medicines until they have had a few years’ experience.
Yes, Myanmar needs more medicine, Dr Aung Zaw said. But it needs high-quality medicine even more. The country’s reliance on global NGOs is a public health concern. Its reliance on the global marketplace is a public health nightmare.
Bad neighbors
Most of the pharmaceutical products in Myanmar come from India, which accounts for twice as much as imports from China and Thailand.
In 2002, the WHO estimated that up to one in five drug products from India were counterfeit. In 2013, Indian pharmaceutical giant Ranbaxy was fined US$500 million in the United States after it was found guilty of misrepresenting clinical generic drug data and selling adulterated drugs to the US.
“India has more than 1000 manufacturers,” Dr Aung Zaw said. “How can we monitor them all?”
High-quality medication from reputable international brands is available in in Myanmar, but public hospitals – which are responsible for buying pharmaceuticals directly from suppliers – usually cannot afford the price.
“We don’t see any problem from our side in terms of supply or quality of product. We do see a problem in price,” said Girish Wadha, president of the Myanmar arm of Thai pharmaceutical maker and distributor, MEGA. The company is one of the largest suppliers to the private healthcare sector, but Mr Wadha said only about five percent of MEGA’s business in Myanmar comes from government tenders.
The only real gatekeeper between these suppliers and public healthcare is the Department of Food and Drug Administration, which has a national workforce of about 400 people but hopes to eventually expand to 2,800 employees, said Dr Win Si Tu, an FDA inspector.
As well as medicines, the FDA is also responsible for overseeing the safety and quality of food and medical devices, for which it has received an almost crippling flood of new products to inspect and register as Myanmar enters the global market. The FDA also keeps a watch out for counterfeit food products and patrols the country’s porous borders in a bid to prevent the smuggling of unregistered medicine.
Dr Win Si Tu said eight to ten percent of the drug samples it tests fail to meet the criteria for registration, and medicines that are approved may decline in quality after entering the market. Companies cut corners on storage and transportation or ease up on good manufacturing practice after a drug has been approved. Ideally, products should undergo routine random checks to ensure sustained quality, but with so few inspectors these tests are few and far between.
This applies to what the FDA is able to test, not the factories where pharmaceuticals are made, many of which are tantalisingly near the wrong side of the border.
The FDA adheres to WHO standards, but labels, credentials, and even entire factories can be faked when companies use phony websites for non-existing plants. Even companies with WHO-approved factories try to sell medicines made at uninspected satellite facilities. “So how can we say this product is really produced by a WHO plant? You can’t trust the label alone.”
U Htoo Myint, CEO of Progress Biochem Co. Ltd. (Ann Wang / Frontier)
Made in Myanmar
When Progress Biochem eventually begins producing, the government will have a real factory to inspect. “It is the easiest way to do quality assurance,” Dr Aung Zaw said.
In return, Progress Biochem and its competitors are not paying tax on construction materials and will not be taxed on the raw materials needed to produce drugs. For the first five years of operation, taxes on production profits will be reduced from 30 percent to zero percent.
“Let’s say we import medicine from Singapore, Malaysia. We can manufacture the exact same quality locally at half of their price,” U Htoo Myint said.
Tax breaks aren’t the only incentive for private players. U Htoo Myint said Myanmar’s transportation and storage infrastructure is a challenge for even the largest middlemen, let alone mid-sized distributors such as Progress. It is relatively difficult to encourage big industry brands to become interested in the Myanmar market, and finding reputable products is only half the battle. It is another matter to sell products in a market flooded with counterfeits.
“[There are] too many identical products in the market; undifferentiated we call it. If you’re talking about paracetamol, there are about 300 brands on the market,” U Htoo Myint said.
The output of the factory remains to be seen, but U Htoo Myint said his company will also source from bigger distributors such as AA Pharmaceuticals and Silver Shine International when their plants are up and running. It should be able to cut its imports by between 50 and 60 percent. It isn’t a transformation, but it is a start.
Yet with Progress Biochem’s new machinery sitting idle, those estimates are still hypothetical. The state-of-the-art facility required imported materials from Singapore and specialists from such countries as Britain and Australia train its pharmacists. The Yangon University alumni have been surprisingly quick learners, U Htoo Myint said, but from the way he described government red tape, building the factory was the easy part.
“When you want to do something there are so many authority concerns,” he said, describing a saga of registrations, proposals and approvals involving the ministries of Health, Finance, Labour, Construction and other branches of the bureaucracy. “There is no coordination at all.”
For example, many of the chemicals needed to test drug samples can also be used to produce illegal narcotics and are tightly controlled. The company has not yet been able to obtain the small amounts needed to test its products and neither has the government offered to conduct the tests. “That’s a problem. Still no solution.”
From scratch
As domestic companies navigate political hurdles, large international drug makers are choosing to bypass Myanmar.
Of the seven aspiring private manufacturers, two are foreign: STADA and DHG, which are German and Vietnamese, respectively. Mr Wadha said that when MEGA decided to increase manufacturing output three years ago, the options were Myanmar or Thailand.
It opted for Thailand, despite the offer of tax incentives. Myanmar axed import tariffs, yes, but countries rarely have high tariffs on drugs.
“Honestly its not as much about location as the quality of the setup that one has,” Mr Wadha said. “It’s not something like a shampoo or a soda where we need to be close to the market to be able to service that market … Maybe somebody is manufacturing in Indonesia or Europe and is supplying half of Asia.”
If the healthcare system wants to end its dependency on shady medicines, it needs to do affordable business with reputable drug makers. Domestic manufacturing operations could drive down costs, but as Mr Wadha explained, Myanmar needs to bring something more to the table than its own market.
“Lets say we manufacture in Thailand. We use that factory for many countries,” he said. “Yes, of course, if you manufacture here you may have some cost advantages now with the duty fees, but one would have to have a broader strategy beyond Myanmar.”
Infrastructure problems are the biggest obstacle to Myanmar becoming an international manufacturing base.
As Progress has already discovered, beyond the challenges involving water, power and roads is a political infrastructure that has never dealt with this sort of thing, said Ben Shoebert from Rubicon Strategy Group, a healthcare consultancy that has worked with the Ministry of Health.
“If you talk about things like drug registration, that whole process, to call it antiquated would be charming,” Mr Shoebert said.
Myanmar has few industry standards of its own or leaders qualified to design them. “In many ways the WHO, UNICEF and groups like that are proxies for the technocratic health administration class that Myanmar just doesn’t have … It’s going to take a really long time to build out the kind of bureaucratic capacity that is going to allow multinationals to efficiently bring products to market.”
Mr Shoebert said manufacturing isn’t the greatest of Myanmar’s public health issues. The troubles with potential manufacturing stem from an overall and developing healthcare system, that is steadily improving.
Even if his company won’t be setting up shop anytime soon, Mr Wadha said that new companies are trying to break into manufacturing at all could be efficacious for healthcare in Myanmar. “These are all greenfield projects … They’re not taking over an existing facility, they aren’t adding a line to an existing facility, they are basically starting manufacturing in Myanmar which was not there before.”
Myanmar may eventually wean itself from foreign drugs, but it won’t be cold turkey.